Documenting Wounds
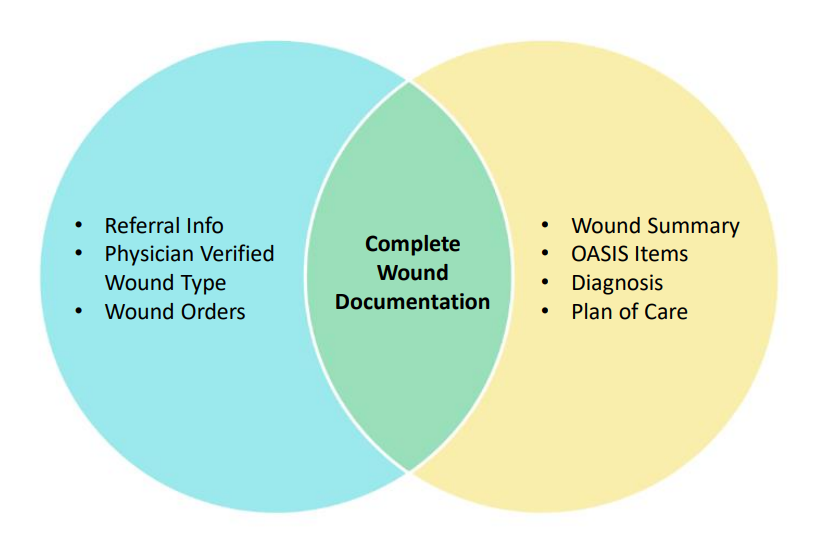
I was honored to present a webinar this past week for the Massachusetts Alliance for Care at Home. Wounds are always tricky, and its great to remind even your seasoned staff about the rules. One of the issues that we see day to day when we are reviewing charts is the lack of consistency in documentation from referral, through to the diagnosis coding, OASIS items, plan of care and wound care orders.
A complete order for wound care includes the following items:
Etiology of Wound
Wound location
Type of wound
Type of cleaning/irrigation solution
Whether skin prep is being used
Type of primary dressing being applied (hydrogel, hydrofiber, calcium alginate, etc.)
Type of secondary dressing being applied, if needed (ABD, border gauze, foam, etc.)
How dressing is being secured (tape, bordered gauze, etc.)
Wound care frequency
Clinicians Can Provide:
Laterality of Wound
Pressure Ulcer Wound Stage
As the highest paid clinical group, its important to get wounds documented correctly! You want to make sure your coders are coding wounds as primary, if appropriate, or secondary to capture the co-morbidity adjustment. 45 of the 98 (46%) comorbidity combinations that result in a high comorbidity adjustment are related to Skin. You need to make sure the eitology of the wound is verified by the physician, and that its the focus of care for it to be captured as primary. If its not the focus of care but its still being cared for or monitored for signs/symptoms of infection, capture it as a second diagnosis. You also want to make sure that your clinicians are documenting the wound in the OASIS items as the same etiology as the physician verified.
If you think your staff need a refresher on wounds, reach out to us. We would be happy to provide your team the education they need.